You are currently browsing the tag archive for the ‘ventilator’ tag.
How Israel Solved the Ventilator Shortage:
Organizing Creativity
By Shlomo Maital
As the world seems to be slowly emerging from the pandemic, fears now turn to a possible second wave. So, we may still need ventilators, in large quantities.
Here is how a creative Israeli team has attacked this problem, according to Rosella Tercatin, writing in the daily Jerusalem Post, May 10:
“Manshema, a $200-a-piece open source technology created by an Israeli team, could solve the problem of the shortage of ventilators crucial to assist patients who contract the most serious forms of COVID-19 worldwide.
“Around mid-March, a group of Israeli organizations – including the IDF, the Assuta Medical Center in Ashdod and Rafael Advanced Technology – engaged several hundreds of their affiliated experts in what they called a “COVID-19 sprint.” The participants were divided into 16 teams to work on finding solutions to a list of problems related to the pandemic. One of the teams decided to tackle the problem of creating a very simple but effective ventilator.
“As explained to The Jerusalem Post by Mordechai Halfon, an officer at the Technological Division of the IDF Ground Forces, within two weeks a first working prototype of the machine was ready.
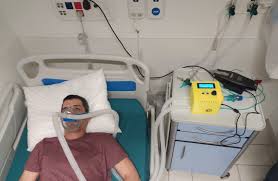
“Our device does not intubate patients, no tube is inserted in their throat to push the air in, they can still breath on their own but the hard work is done by the machine,” he said. “It is catered specifically to COVID-19 patients, who required a very specific type of ventilation. This is why it is so simple, as opposed to regular ventilators which need to be suitable for many different kinds of needs.”
“The Manshema team includes different kind of engineers, medical experts, product managers, who had never met before. Seven of them have been working on the project full time – Gil Bachar, Stav B., Elad Grozovski, Ronen Zilberman, Roi Galili Darnell, Ivry Shapira, Omri Mizrachi – others are contributing in different capacities.
“At the beginning, the group worked on the task by themselves, meeting online when required. Afterwards, they started to meet at the Tel Aviv branch of Assuta.
“The project is completely nonprofit and opensource, which means that all the relevant information is available to any manufacturer interested in producing them or medical center in using them all over the world.”
Coronavirus: Cheap Israeli technology may solve world ventilator shortage
The project is completely nonprofit and opensource.
By ROSSELLA TERCATIN
MAY 10, 2020 17:
“Because we are talking about a world-wide pandemic, it was important for the ventilator to be cheap and easy to manufacture. We also wanted it to be disposable,” Stav B., a doctoral student at the Tel Aviv University, told the Post. “Quite at the beginning, we were selected by the Health Ministry as a pilot project and they supported us.”
Since the cost of production of every unit stands at about $200 and the time required at around two/three hours of work, while ventilators available to the market cost from several thousands to several dozen thousand dollars and have become harder and harder to find and purchase, the product could really revolutionize the fight against the virus even in the poorest countries.
“We have received a lot of support also from many companies here in Israel. We have found out that since nobody is involved in the initiative to make money, everyone has been very happy to help us in providing what we needed just for the goal of fighting the virus,” Halfon explained.
The product will undergo clinical trials at Assuta Medical Center in the next few weeks.
“In the first phase, we are going to test it on healthy volunteers, which should be easy to find, after on patients and critical patients. We are not sure how long it will take to complete the trial, but we are hoping that we are going to be ready before the next wave of the virus, if it comes,” the captain pointed out. “We believe that this machine can save a lot of lives.”
Halfon explained that when everything started, they did not think they would be able to arrive to this point.
“We worked through steps. First, we decided to dive into the actual requirements that the machine would need, then we focused on how the solution would look in a broader perspective and only then on how to build the machine,” he said.
“I think it is important to highlight two key elements in our work: the quality of the team effort and the will to do something good,” he concluded.
Getting Ahead of COVID-19: Dr. Levitan’s Wisdom
By Shlomo Maital
Dr. Richard Levitan, holding a pulse oximeter
Dr. Richard Levitan is an emergency medicine doctor, specializing in respiration, and normally practices medicine at a small hospital in Littleton Regional Healthcare, Littleton, New Hampshire. When the coronavirus pandemic broke out, he volunteered to help doctors at Bellevue Hospital in New York City, where he once trained.
He has many valuable insights on how we must change the way we treat this disease, based on his professional experience and knowledge, and on what he saw at Bellevue. His article appears on CNN’s website. Here is a short version. Again, I apologize for this 1,850 word blog… but I felt all Levitan’s words were important.
The bottom line: Use a simple device, an oximeter, to detect when oxygen levels are low, indicating virus distress, and start THEN to treat the patient, long before a ventilator is needed. The body adjusts, and breathes more rapidly, so often people ill with coronavirus do not call for medical help until they are very far gone and their lungs have serious pneumonia. Many do not recover even when ventilated, and those that do, often need dialysis or have blood clots.
….
“I have been practicing emergency medicine for 30 years. In 1994 I invented an imaging system for teaching intubation, the procedure of inserting breathing tubes. This led me to perform research into this procedure, and subsequently teach airway procedure courses to physicians worldwide for the last two decades.
“So at the end of March, as a crush of Covid-19 patients began overwhelming hospitals in New York City, I volunteered to spend 10 days at Bellevue, helping at the hospital where I trained. Over those days, I realized that we are not detecting the deadly pneumonia the virus causes early enough and that we could be doing more to keep patients off ventilators — and alive.
“On the long drive to New York from my home in New Hampshire, I called my friend Nick Caputo, an emergency physician in the Bronx, who was already in the thick of it. I wanted to know what I was facing, how to stay safe and what his insights into airway management with this disease were. “Rich,” he said, “it’s like nothing I’ve ever seen before.”
“He was right. Pneumonia caused by the coronavirus has had a stunning impact on the city’s hospital system. Normally an E.R. has a mix of patients with conditions ranging from the serious, such as heart attacks, strokes and traumatic injuries, to the non-life-threatening, such as minor lacerations, intoxication, orthopedic injuries and migraine headaches.
“During my recent time at Bellevue, though, almost all the E.R. patients had Covid pneumonia. Within the first hour of my first shift I inserted breathing tubes into two patients. Even patients without respiratory complaints had Covid pneumonia. The patient stabbed in the shoulder, whom we X-rayed because we worried he had a collapsed lung, actually had Covid pneumonia. In patients on whom we did CT scans because they were injured in falls, we coincidentally found Covid pneumonia. Elderly patients who had passed out for unknown reasons and a number of diabetic patients were found to have it.
“And here is what really surprised us: These patients did not report any sensation of breathing problems, even though their chest X-rays showed diffuse pneumonia and their oxygen was below normal. How could this be? We are just beginning to recognize that Covid pneumonia initially causes a form of oxygen deprivation we call “silent hypoxia” — “silent” because of its insidious, hard-to-detect nature.
“Pneumonia is an infection of the lungs in which the air sacs fill with fluid or pus. Normally, patients develop chest discomfort, pain with breathing and other breathing problems. But when Covid pneumonia first strikes, patients don’t feel short of breath, even as their oxygen levels fall. And by the time they do, they have alarmingly low oxygen levels and moderate-to-severe pneumonia (as seen on chest X-rays). Normal oxygen saturation for most persons at sea level is 94 to 100 percent; Covid pneumonia patients I saw had oxygen saturations as low as 50 percent.
“To my amazement, most patients I saw said they had been sick for a week or so with fever, cough, upset stomach and fatigue, but they only became short of breath the day they came to the hospital. Their pneumonia had clearly been going on for days, but by the time they felt they had to go to the hospital, they were often already in critical condition.
“In emergency departments we insert breathing tubes in critically ill patients for a variety of reasons. In my 30 years of practice, however, most patients requiring emergency intubation are in shock, have altered mental status or are grunting to breathe. Patients requiring intubation because of acute hypoxia are often unconscious or using every muscle they can to take a breath. They are in extreme duress. Covid pneumonia cases are very different.
“A vast majority of Covid pneumonia patients I met had remarkably low oxygen saturations at triage — seemingly incompatible with life — but they were using their cellphones as we put them on monitors. Although breathing fast, they had relatively minimal apparent distress, despite dangerously low oxygen levels and terrible pneumonia on chest X-rays.
“We are only just beginning to understand why this is so. The coronavirus attacks lung cells that make surfactant. This substance helps the air sacs in the lungs stay open between breaths and is critical to normal lung function. As the inflammation from Covid pneumonia starts, it causes the air sacs to collapse, and oxygen levels fall. Yet the lungs initially remain “compliant,” not yet stiff or heavy with fluid. This means patients can still expel carbon dioxide — and without a buildup of carbon dioxide, patients do not feel short of breath.
“Patients compensate for the low oxygen in their blood by breathing faster and deeper — and this happens without their realizing it. This silent hypoxia, and the patient’s physiological response to it, causes even more inflammation and more air sacs to collapse, and the pneumonia worsens until oxygen levels plummet. In effect, patients are injuring their own lungs by breathing harder and harder. Twenty percent of Covid pneumonia patients then go on to a second and deadlier phase of lung injury. Fluid builds up and the lungs become stiff, carbon dioxide rises, and patients develop acute respiratory failure.
“By the time patients have noticeable trouble breathing and present to the hospital with dangerously low oxygen levels, many will ultimately require a ventilator. Silent hypoxia progressing rapidly to respiratory failure explains cases of Covid-19 patients dying suddenly after not feeling short of breath. (It appears that most Covid-19 patients experience relatively mild symptoms and get over the illness in a week or two without treatment.)
“A major reason this pandemic is straining our health system is the alarming severity of lung injury patients have when they arrive in emergency rooms. Covid-19 overwhelmingly kills through the lungs. And because so many patients are not going to the hospital until their pneumonia is already well advanced, many wind up on ventilators, causing shortages of the machines. And once on ventilators, many die.
“Avoiding the use of a ventilator is a huge win for both patient and the health care system. The resources needed for patients on ventilators are staggering. Vented patients require multiple sedatives so that they don’t buck the vent or accidentally remove their breathing tubes; they need intravenous and arterial lines, IV medicines and IV pumps. In addition to a tube in the trachea, they have tubes in their stomach and bladder. Teams of people are required to move each patient, turning them on their stomach and then their back, twice a day to improve lung function.
“There is a way we could identify more patients who have Covid pneumonia sooner and treat them more effectively — and it would not require waiting for a coronavirus test at a hospital or doctor’s office. It requires detecting silent hypoxia early through a common medical device that can be purchased without a prescription at most pharmacies: a pulse oximeter.
“Pulse oximetry is no more complicated than using a thermometer. These small devices turn on with one button and are placed on a fingertip. In a few seconds, two numbers are displayed: oxygen saturation and pulse rate. Pulse oximeters are extremely reliable in detecting oxygenation problems and elevated heart rates.
“Pulse oximeters helped save the lives of two emergency physicians I know, alerting them early on to the need for treatment. When they noticed their oxygen levels declining, both went to the hospital and recovered (though one waited longer and required more treatment). Detection of hypoxia, early treatment and close monitoring apparently also worked for Boris Johnson, the British prime minister.
“Widespread pulse oximetry screening for Covid pneumonia — whether people check themselves on home devices or go to clinics or doctors’ offices — could provide an early warning system for the kinds of breathing problems associated with Covid pneumonia. People using the devices at home would want to consult with their doctors to reduce the number of people who come to the E.R. unnecessarily because they misinterpret their device. There also may be some patients who have unrecognized chronic lung problems and have borderline or slightly low oxygen saturations unrelated to Covid-19.
“All patients who have tested positive for the coronavirus should have pulse oximetry monitoring for two weeks, the period during which Covid pneumonia typically develops. All persons with cough, fatigue and fevers should also have pulse oximeter monitoring even if they have not had virus testing, or even if their swab test was negative, because those tests are only about 70 percent accurate. A vast majority of Americans who have been exposed to the virus don’t know it.
“There are other things we can do as well to avoid immediately resorting to intubation and a ventilator. Patient positioning maneuvers (having patients lie on their stomach and sides) open up the lower and posterior lungs most affected in Covid pneumonia. Oxygenation and positioning helped patients breathe easier and seemed to prevent progression of the disease in many cases. In a preliminary study by Dr. Caputo, this strategy helped keep three out of four patients with advanced Covid pneumonia from needing a ventilator in the first 24 hours.
“To date, Covid-19 has killed more than 40,600 people nationwide — more than 10,000 in New York State alone. Oximeters are not 100 percent accurate, and they are not a panacea. There will be deaths and bad outcomes that are not preventable. We don’t fully understand why certain patients get so sick, or why some go on to develop multi-organ failure. Many elderly people, already weak with chronic illness, and those with underlying lung disease do very poorly with Covid pneumonia, despite aggressive treatment.
“But we can do better. Right now, many emergency rooms are either being crushed by this one disease or waiting for it to hit. We must direct resources to identifying and treating the initial phase of Covid pneumonia earlier by screening for silent hypoxia.
“It’s time to get ahead of this virus instead of chasing it.”
Creativity Is the Answer: Oxford’s New Ventilator!
By Shlomo Maital
Prof. Andrew Farmery OxVent: simple, effective
In times of crisis, like the ones we are living today, resources and time are scarce – but creativity is plentiful. For example: Creative British doctors and scientists who have designed a primitive, simple, easy-to-produce ventilator, which SONY may mass produce. NY Governor Andrew Cuomo said today that his state has 10,000 ventilators, but it needs 30,000, as the coronavirus is spreading rapidly in his state – and the US Federal Govt. (FEMA) has sent…400 of them, even though there are 20,000 of them in an emergency US stockpile.
[A ventilator is a device that pumps air into the lungs of coronavirus victims, who struggle to breathe].
Here is the story.
Interviewer: “In just one week, a team at Oxford University and King’s College London have built a simple ventilator that could potentially save thousands of lives as part of the UK and the world’s fight against coronavirus. The OxVent is a rapid prototype ventilator that could keep people breathing while they battle the worst impacts of COVID-19. Andrew Farmery of the University of Oxford, one of the people involved in its development, talks about its past, present, and potential. … How are you?
Prof. Andrew Farmery: ” I’m very well, although slightly knackered. It’s been a very long week. It’s been absolutely incredible, from nothing a week ago when we first had an idle chat Monday morning last week, to this afternoon, when we pitched it to the Cabinet and the MHRA (Medicines and Healthcare Products Regulatory Agency). We’re waiting to hear whether they think it’s a goer or not.”
Farmery: “It’s laughably simple in some ways. It’s a compressible bag, a bit like a child’s rugby ball. It’s a compressible squeezy bag – the sort you use to resuscitate patients who have collapsed from cardiac arrest. Ambulances carry them around. But we’ve trapped it inside a rigid Perspex box and we inject compressed air into the rigid Perspex box that squeezes this bladder and pushes air out through some valves which we already have, and inflates the patient’s chest. There’s a second set of valves that allows gas to come out of the patient’s chest and also out of the rigid Perspex box. So it’s a sort of electro-pneumatic device. The air is injected into the box through what’s called a solenoid valve, which is controlled electronically, and we can regulate the flow of air compression gas that goes into the box, the speed with which it goes in, how much time is allowed for inspiration and expiration. We can control the pressures generated in the patient’s airway. All the things you would want, and we’re just doing it with this simple feedback controller.”
Farmery continues: “As well as an academic, I’m also a consultant anaesthetist, so I deal with ventilating patients every week. That’s what I do. The design had come out of what the clinicians want. We were slightly worried at the start when Boris [Johnson, UK PM] announced Land Rover and JCB were going to be making ventilators. I was slightly alarmed that they knew sod-all about ventilators and nobody had really taken the opinions of people like me and doctors and anesthetists around the country.”
“The electronics is based around a very simple circuit board called an Arduino – basically a tiny little circuit board used to teach kids about coding and electronics. It’s basically a toy, but that’s what the prototype is based on. We might even base the whole thing on that. It depends on whether we can knock PCBs out quickly enough. So the control engineers are still working on that, refining it. You’ve got to tell the solenoid valve what to do and then you’ve got to measure and monitor the pressures at various points with sensors to make sure that the solenoid is doing what you told it to do. That’s classic control engineering and they love that sort of thing, and they’re off on it already.”
SONY is exploring the possibility of making 5,000 of the new ventilators weekly I hope the design can be shared with other countries, including my own, Israel.